Key takeaways
- Communication comes in many forms. Non-verbal communication is challenging but absolutely critical to patient-doctor relationships.
- A good communicator would consider any potential physical limitations or cultural differences that can prevent or obstruct communication.
- Without efficient communication skills, achieving patient-centred care, shared decision-making, and interprofessional collaboration is very limited.
- Emotional intelligence helps healthcare professionals better comprehend, involve, and inspire the people around them. They are necessary for resolving conflict and creating practical solutions to complex problems that can arise in the healthcare environment.
- Through secure collaboration and evaluation, Videolab improves self-awareness, decision-making, and self-confidence resulting in clarity in communication and intention
What is communication?
By definition, communication is “the activity or process of expressing ideas and feelings or of giving people information”
Essentially, communication is any basic exchange of information by any means. Everyone communicates differently, which is where the teaching and learning of the ‘correct communication’ can be tricky.
In this blog, we discuss the basics of different communication skills, patient centred care and emotional intelligence. In today’s complex healthcare environment, teaching students how to think critically and communication efficiently is crucial. Our product Videolab specifically targets these teaching areas by leveraging modern feedback mechanisms with medical education and privacy by design principles in mind.
Communications skills in healthcare
Communication is the foundation of quality healthcare and patient safety, every healthcare professional needs a certain level of good communication skills. Effective communication skills positively impact patients and the team around you, resulting in better patient outcomes and a successful work environment.
Throughout a communication exchange, there is a level of meaning loaded in the message, what this meaning is, depends entirely on the situation, however for a transfer of communication to be successful, both parties must agree on the meaning of what is being communicated.
Continuing further, a good communicator would consider any potential physical limitations or cultural differences that can prevent or obstruct communication. According to (Mccorry, K.L., Mason, J. 2020), the communication process can be shown in five steps:
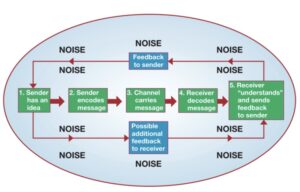
Image retrieved from: Mccorry, K.L., Mason, J. (2020) Communication Skills for the Healthcare Professional, Enhanced Edition. Jones & Barlett Learning.
Noise in Communication
Noise represents any communication that hinders the message being received. The level of noise a healthcare provider uses can depend on many aspects such as;
- The difficulty of the message being transmitted. (e.g. bad news) Therefore trying to avoid any silence.
- The receiver may be distracted by fear or anxiety about the message being communicated.
- Language barriers that prevent understanding of the message.
- The message may be very technical in terms of medical diagnosis, too much noise can be communicated to try to simplify the message to the receiver.
This language is typically used to ‘soften the blow’ of bad news, however, in a healthcare setting, noise impedes the actual meaning of the message and can cause the receiver confusion. Noise disrupts the communication process and must be avoided at all times.
Nonverbal communication
Nonverbal communication cues, such as the way you listen, look, move and respond, let the person you’re speaking with know whether or not you care, whether you’re being truthful and how attentive you are.
Types of nonverbal communication include:
- Facial expressions
- The human face is incredibly expressive and can silently reflect a wide range of emotions.
- Body movement and posture
- A person’s posture, gait, head position, and arm gestures can influence how you see or feel about them. The world can learn a lot about you from the way you move and carry yourself.
- Gestures
- Our daily lives are made up of gestures in one way or another. When debating or explaining ourselves, we might wave, point or use our hands to express ourselves without giving them any thought. However, we must take into account that some gestures can be different across cultures.
- Eye contact
- Eye contact is an especially important type of nonverbal communication, the way you look at someone can convey a variety of emotions, such as attention, affection, hatred, annoyance, or attraction. Maintaining eye contact is crucial for the flow of a discussion and for determining the other person’s level of attention.
- Touch
- We communicate a great deal through touch, different messages can be conveyed through different sources of touch, for example; a strong or weak handshake, a big warm hug or a touching or grazing of the arm, or a controlling grip of the arm can all communicate different messages and leave impressions on the receiver.
- Space
- Have you ever experienced awkwardness during a conversation because the other person was invading your personal space? Although our needs for physical space vary depending on culture or circumstance, the need is still there. Physical space can be used to convey a variety of nonverbal cues, such as expressions of intimacy or affection, dominance, or hostility.
The difficulty of nonverbal communication is that it occurs simultaneously, generally, it’s not something that we have under such control, the cognitive control is given and reveals more of what we actually think and feel. Therefore, it can be harder to manage and anticipate compared to verbal communication, which, with less practice than nonverbal, is done intentionally and is easier to manipulate. Due to this, we usually pick up quicker on nonverbal cues and have more trust in the information or intention. For instance, the recipient is more likely to trust the nonverbal signal when having a discussion with a person that is telling you one thing out loud but unconsciously conveys a different message non-verbally.
Nonverbal and verbal communication should compliment each other. Its essential healthcare and social care providers have situational awareness to recognize potential appropriate or inappropriate body language in a patient consultation.
The ability of students, doctors, nursing, and all healthcare providers to understand nonverbal communication in correlation with verbal communication is a very powerful tool. This aids the connection with patients and reinforces a strong relationship between patient and provider.

What is patient-centered care?
Patient-centered care encourages active collaboration and shared decision-making between patients, families, and providers.
Its objective is to strengthen patient empowerment and allow patients to gain greater control over decisions and actions relating to their health. World Health Organisation. (2009).
In order to reach this goal, patients should feel heard and understood by their provider, those who do, are more motivated to take action and do what is necessary to recovery and therefore have a higher likelihood of a positive health outcome.
Empowered patients are more enthusiastic about their care and, or ready to understand and learn what they should do to recover and continue with a healthy lifestyle. Empathy and soft skills are what help patients feel they are receiving high-quality care with a healthcare provider they can trust and work together with.
Emotional intelligence
Skills in emotional intelligence (EI) help healthcare professionals better comprehend, involve and inspire the people around them. They are necessary for resolving conflict and creating practical solutions to complex problems that can arise in the healthcare environment.
Emotional intelligence skills are built on the foundation of personal competence, which can then allow an individual to improve skills of social competence, such as soft skills, empathy and relationship building. A company’s organizational culture can be significantly impacted by the qualities a leader possesses, emotional intelligence being a big factor in this.
Healthcare is a challenging work environment due to the pure complexities of the field, there are many factors to be considered when dealing with each patient, going from the patient background and family situation to regulatory convolution and diagnosis and treatment.
Nowadays, more attention is paid to communication skills and soft skills training in healthcare. More universities have added specific classes to their curriculum and the general standard for these skills is set higher.
However, in terms of evaluation and measurement of EI skills in students, it still presents challenges due to the complexity of the skill. Assessments that determine a student’s EI ability are not available in the same sense as clinical evaluations of students. EI assessments are approached in a more generalized analysis of these personal and social competencies.
How to improve your communication skills?
Improving communication skills is a long-term task and something we should be working on continuously. There are many ways in which one can improve these skills, one study suggested the following tips.
Five NHS clinicians working across primary and secondary care were asked for advice on how to communicate efficiently in difficult healthcare situations. Their practical tips were as follows.
- Be attentive: Listen to what your patient is saying rather than thinking about the next question or possibly already presuming their symptoms and diagnosis.
- Ask open questions: Open-ended questions allow respondents to include more information giving you more useful and contextual information.
- Be curious: Maintaining curiosity about a patient will increase interest and investigation of the core issue or problem.
- Summaries throughout: Summarising the information being spoken the way through a consultation assures both patient and doctor have correctly understood key points.
- Involve friends and family: Under stressful or anxious situations, such as in many healthcare environments can affect the memory or full understanding of what’s going on for a patient. Involving family or friends can help them reflect and explore their options.
- Use the right tone: Using the right tone is extremely important for the communication process. The language a doctor uses should be appropriate to the situation and can affect patient-centered care immensely
- Be aware of your patient’s situation: Every patient is different and every situation is different, providers must try to understand and empathize by using different management techniques.
- Get help from colleagues: Second opinions can be very useful, especially in the seriousness of a healthcare situation, it can also help patients feel more comfortable if there are more doctors to help them.
- Be aware of bias: Healthcare professionals must be able to acknowledge their personal biases, and deal with them accordingly to ensure they do not affect the care given to patients.
- Communicate in different ways: There are many diverse ways to communicate which can make the message being communicated more effective. Exploring different communication tools can be a useful technique for healthcare providers.
- Adopt share decision making: This relates to patient-centred care, if your patient feels included in their health journey, they are likely to be more engaged and positive towards their recovery. This will also build a stronger relationship between patient and doctor.
- Try active listening: Active listening encourages openness, honesty and success. You allow the other person to feel they are being heard and understood, this is a huge factor in communication that helps build trust.
- Watch yourself back: If recordings are allowed in a consultation, they can be a huge aid towards reflecting upon your own performance and improving from this.
- Speak up: Building an environment within your team where everyone feels they are able to speak up, be open and share ideas can allow a lot of room for learning and improvement.
How can Videolab help develop skills of communication?
Videolab is a privacy-compliant video sharing platform where you are able to record patient interactions in a GDPR-safe environment.
Trainees are able to upload simulated consultations, peer consultation or real patient consultation which are encrypted once the upload is complete. Students are then able to go back and watch this recording, reflect on their performance,
make time fragmented comments or ask questions. These recordings are then shared with pre approved assessors to mark and evaluate. Secure collaboration also allows students to securely share the recording with peers and receive feedback from multiple different sources. Videolab can specifically address the issue when accessing emotional intelligence as it allows for a complex and diverse evaluation environment.
Videolab is a MedTech solution that allows for secure healthcare training and has many use cases, Codific believes in adapting the application to your use case. Thus, it is particularly useful for the training of soft skills and communication training during patient interactions. Hence, Videolab is very practical and effective to improve communication skills, empathy training, nonverbal communication etc….
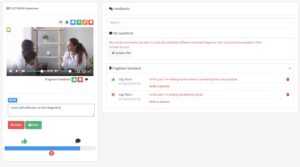
The act of watching a consultation back is a very powerful tool, self-reflection in education is an essential element that aids self-awareness increases emotional intelligence, and our capacity to recognize the results of our actions. Self-awareness helps decision-making, subsequently increasing self-confidence and furthermore resulting in clarity in communication and intention.
What else does Codific build with privacy by design principles?
Codific is a team of security software engineers that leverage privacy by design principles to build secure cloud solutions. We build applications in different verticals such as HR-tech, Ed-Tech and Med-Tech. Secure collaboration and secure sharing are at the core of our solutions.
SAMMY Is a Software Assurance Maturity Model management tool. It enables companies to formulate and implement a security assurance program tuned to the risks they are facing. That way other companies can help us build a simple and safe digital future.
We believe in collaboration and open innovation, we would love to hear about your projects and see how we can contribute in developing secure software and privacy by design architecture. Contact us.
References:
Berkovic, E. (SSSS) The importance of non-verbal communication. Marbella International University Centre. https://miuc.org/importance-of-non-verbal-communication/
Chan, S. (2020). 16 ways to improve your communication skills with patients. British Heart Foundation. https://www.bhf.org.uk/for-professionals/healthcare-professionals/blog/16-ways-to-improve-your-communication-skills-with-patients
Fernandez, C., Peterson, H., Holmstrom, S., Connolly, A. (2011) Developing Emotional Intelligence for Healthcare Leaders. The University of North Carolina and Chapel Hill, The University of South Florida,
Mccorry, K.L., Mason, J. (2020) Communication Skills for the Healthcare Professional, Enhanced Edition. Jones & Barlett Learning. https://books.google.be/books?hl=en&lr=&id=TaLqDwAAQBAJ&oi=fnd&pg=PP1&dq=communication+skills+in+healthcare&ots=zFhk4etpDc&sig=dWupHk3pJdQF80-M1K2-gqWvvYI#v=onepage&q=communication%20skills%20in%20healthcare&f=false
Segal, J., Smith, M., Robinson, L., Boose, G. (2020) Nonverbal Communication and Body Language. Help Guide. https://www.helpguide.org/articles/relationships-communication/nonverbal-communication.htm

