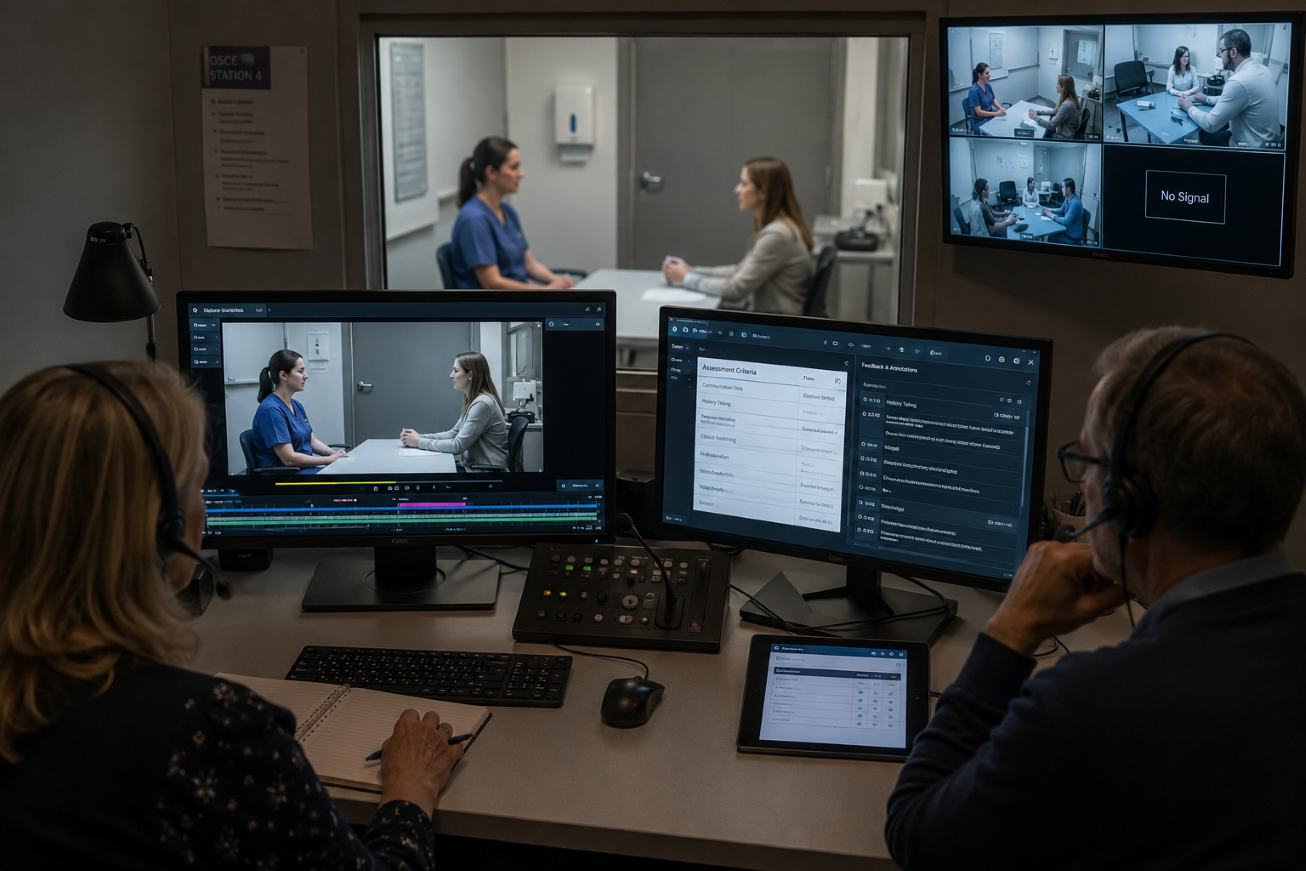
Medical faculties rarely struggle to record video. The difficult part is managing what happens afterwards. Clinical skills training often involves multiple assessors, sensitive recordings, structured feedback, and long term competency tracking. A generic recording platform may capture the interaction, but it usually does not support the educational workflow around it.
This becomes particularly visible in OSCEs, simulation based education, and workplace assessments. Educators need to review recordings efficiently, control access to sensitive material, provide timestamped feedback, and retain evidence in line with institutional and GDPR requirements.
As a result, choosing video recording software for medical education is less about image quality and more about governance, assessment workflows, and educational usability. This article outlines seven requirements medical faculties should evaluate before selecting a platform.
Most medical faculties do not need a generic recording tool
Medical faculties usually need more than a platform that can capture and store video. Clinical education workflows involve assessment, structured feedback, controlled sharing, and long term review across multiple users and departments. Generic recording tools rarely support these processes in a reliable way.
This limitation often appears gradually. A faculty may initially use consumer video platforms because they are already available institution wide. Over time, educators begin relying on spreadsheets to track assessments, external messaging tools to coordinate feedback, or downloaded video files to manage reviews manually. The recording tool becomes disconnected from the educational workflow surrounding it.
Clinical training environments also introduce governance requirements that are less common in general education settings. Recordings may contain patient interactions, simulated consultations, or identifiable learner performance data. Faculties therefore need clear access controls, retention policies, and auditability. Under the General Data Protection Regulation (GDPR), compliance depends on how data is managed across the entire workflow, not only where the file is stored.
Specialized platforms are designed around these operational realities. Rather than treating video as standalone content, they support structured educational review, assessment processes, and secure collaboration between learners, assessors, and program administrators.
For a broader comparison between general purpose and healthcare specific platforms, see Generic vs Specialized Video Tools for Healthcare Settings.
Clinical education workflows place different demands on recording software
Clinical education workflows depend on structured observation and review, not simply video capture. Recording software used in medical faculties therefore needs to support assessment processes that extend beyond standard meeting or lecture recording.
OSCE review and examiner assessment
In OSCE environments, recordings are often reviewed by multiple examiners across different stations or assessment cycles. Educators may need to revisit performances for moderation, examiner calibration, appeals, or quality assurance. This requires consistent organization, controlled access, and reliable retrieval of recordings.
Video based rating can also improve operational flexibility during OSCEs. Research on video based examiner workflows found that assessments and examiner reviews no longer need to occur simultaneously, reducing scheduling pressure and allowing assessors to focus on a smaller set of standardized evaluation tasks.
Additional context on OSCE workflows can be found in Getting Started with Video Based OSCEs.
Simulation and debriefing
Simulation programs often use video during debriefing because learners may not accurately recall their own behavior during a scenario. Reviewing selected moments allows facilitators to discuss communication patterns, clinical reasoning, teamwork, and decision making with greater precision.
Structured video review during debriefing allows facilitators to revisit communication, teamwork, and clinical reasoning with greater precision than memory based discussion alone.
For more on structured debriefing approaches, see Effective Debriefing Models for Simulation Based Medical Education.
Workplace based assessment and EPAs
Many competency based programs now use longitudinal assessment models that collect evidence over time rather than relying exclusively on high stakes examinations. Video recordings can contribute to this process by documenting learner performance across different clinical encounters.
Entrustable Professional Activities, commonly referred to as EPAs, often depend on repeated observation and feedback across multiple assessors and settings. Recording systems used in these environments need to support organized review, contextual feedback, and long term evidence management.
The Association of American Medical Colleges describes workplace based assessment as a central component of competency based medical education.
GDPR compliance is not only about storage location
Many platforms describe themselves as GDPR compliant because their servers are located in Europe. In practice, compliance depends on how personal data is accessed, shared, retained, and governed throughout the educational process.
Medical education recordings may contain identifiable patient information, student assessment data, or sensitive communication scenarios. Faculties therefore need to consider who can access recordings, whether downloads are restricted, how retention periods are managed, and whether activity can be audited when concerns arise.
Under the GDPR, organizations must implement appropriate technical and organizational measures to protect personal data. This includes access control, data minimization, and secure processing practices. A recording platform that allows unrestricted file downloads or informal sharing may create governance problems even if the underlying storage infrastructure is European.
Consent management also becomes important in environments involving simulated patients, workplace assessment, or recorded clinical encounters. Faculties need clear processes that define who can review recordings, how long they remain accessible, and when they should be deleted.
More detailed guidance is available in GDPR Compliance for Healthcare Facilities.
Seven features medical faculties should evaluate before choosing a platform
Medical faculties should evaluate recording platforms based on workflow support and governance requirements, not only recording quality or storage capacity. The most useful systems reduce operational complexity around assessment and feedback.
- Role based permissions
Different users require different levels of access. Learners, assessors, administrators, and external examiners should not automatically see the same material. - Structured timestamp feedback
Feedback linked directly to specific moments in a recording is easier for learners to interpret and revisit during reflection or remediation. - Controlled sharing and download restrictions
Institutions should be able to define how recordings are shared and whether local downloads are permitted. - Assessment workflow support
Platforms used for OSCEs or workplace based assessment should support structured review rather than functioning only as passive storage systems. - Retention and deletion controls
Medical faculties often need defined retention schedules for assessment material and simulated patient recordings. - Auditability
Administrators may need visibility into who accessed a recording, when it was reviewed, and whether it was shared externally. - Reliable multi device recording
Clinical education environments are operationally unpredictable. Recording systems need to function consistently across simulation rooms, consultation spaces, and mobile setups.
These requirements become more important as programs scale across multiple cohorts, departments, or clinical sites.
Consumer video platforms create hidden operational problems
Consumer video platforms usually fail when medical faculties need structured assessment, governance, and coordinated review workflows.
One common issue is workflow fragmentation. Recordings may exist in one system, assessment forms in another, and feedback conversations in email threads or spreadsheets. Educators then spend time coordinating material manually instead of reviewing learner performance.
This fragmentation becomes more difficult to manage as programs scale across multiple cohorts or assessment sites. Recording based tools are now the most commonly used digital modality in communication skills education, according to a 2026 scoping review of medical education technologies.
Video review works best when feedback is structured
Video review becomes educationally useful when learners receive specific and structured feedback linked to observable behavior. Simply watching a recording rarely improves performance on its own.
A 2024 meta analysis covering 40 studies reported moderate to large improvements in clinical skills, knowledge acquisition, and professional attitudes across video based health education interventions. The strongest outcomes were observed when video review was paired with structured feedback, reflection prompts, or guided assessment frameworks.
Structured review allows educators to direct attention toward particular communication behaviors, clinical decisions, or teamwork interactions. Timestamped comments are especially useful because learners can revisit exact moments rather than relying on general recollection after the encounter.
Studies on video based feedback consistently report that learners identify communication behaviors and performance gaps they did not notice during the original interaction.
Peer feedback can become more consistent as well. When learners review the same interaction using shared criteria, discussions tend to focus more on observable behavior and less on vague impressions. This is particularly relevant in communication skills training, simulation debriefing, and workplace based assessment.
For additional perspectives on structured feedback approaches, see Formative vs Summative Feedback and Peer Feedback in Medical Education.
Conclusion
Choosing video recording software for medical education involves evaluating how the platform supports assessment, feedback, governance, and long term educational review. Recording quality alone is rarely the deciding factor in clinical training environments.
As programs expand across simulation, OSCEs, workplace based assessment, and competency based curricula, operational requirements become increasingly difficult to manage through disconnected consumer tools and manual review workflows.
We have designed Videolab specifically for these healthcare education environments. Rather than functioning as a general purpose recording platform, it supports structured feedback, secure review workflows, and assessment processes used in clinical skills training and professional education programs.