What is empathic accuracy
Empathic accuracy is the ability to correctly infer another person’s thoughts and feelings in a specific moment. It differs from general empathy by focusing on how precise that understanding is, rather than how much emotional connection or concern a person shows.
In clinical communication, this distinction is critical. Clinicians often rely on a sense of understanding that feels accurate. However, that perception does not guarantee that their interpretation matches what the patient actually thinks or feels. Empathic accuracy instead requires alignment between inference and the patient’s internal state.
Definition and origin of the concept
The concept comes from research on interpersonal perception. It describes everyday attempts to “read” another person’s thoughts and emotions and evaluates how successful those attempts are. This makes empathic accuracy a measurable outcome rather than a general trait.
Studies assess this by comparing what one person believes another experienced with what that person reports. This comparison reveals whether understanding is correct, partially correct, or inaccurate.
How it differs from empathy
Empathy focuses on emotional engagement. A clinician may feel concerned, attentive, or supportive. However, these responses do not indicate whether the clinician has interpreted the patient correctly.
Empathic accuracy focuses on interpretation. It asks whether the clinician understood what the patient actually meant, felt, or intended. As a result, a clinician can appear empathic while still misunderstanding the patient.
Why accuracy matters in clinical settings
Clinical decisions often depend on interpretation. Misunderstanding a patient’s concern, priority, or emotional state can affect diagnosis, communication, and trust.
Because internal states are not directly observable, clinicians must rely on cues and inference. This makes accuracy uncertain. Therefore, empathic accuracy should be treated as a variable that can fail, rather than as a given outcome of good communication.
This leads to a practical question: why do clinicians misread patients even when they are attentive and engaged?
Why clinicians misread patients
Clinicians misread patients because empathic accuracy depends on inference under uncertainty. Even when communication appears effective, the underlying interpretation may still be incorrect.
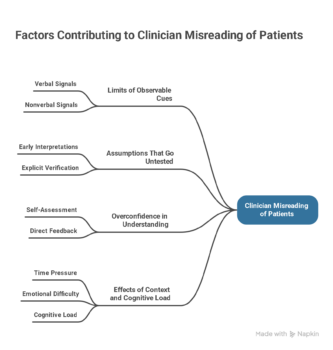
Limits of observable cues
Patients communicate through a mix of verbal and nonverbal signals. However, these signals are often subtle or ambiguous. A pause may indicate hesitation, reflection, or discomfort. Without context, interpretation becomes uncertain.
Clinicians must select which cues matter. When important signals are missed or misinterpreted, the resulting understanding is incomplete.
Assumptions that go untested
During consultations, clinicians often form early interpretations. These interpretations guide the rest of the interaction. However, they are not always tested or confirmed.
Without explicit verification, incorrect assumptions can persist. Over time, they shape how clinicians respond, even when the patient provides conflicting information.
Overconfidence in understanding
Research shows that individuals are not reliable judges of their own empathic accuracy. They may believe they understand another person even when their interpretation is incorrect.
This creates a gap between perceived and actual understanding. In clinical settings, this gap can remain invisible because there is no direct feedback on accuracy.
Effects of context and cognitive load
Empathic processes vary depending on context. Time pressure, emotional difficulty, and cognitive load all affect how clinicians interpret patient information.
Under these conditions, clinicians may rely more on shortcuts or prior assumptions. As a result, the likelihood of misinterpretation increases.
These factors show that misreading patients is not an exception. It is a predictable outcome of how empathic accuracy works. This raises a key distinction that often goes unnoticed: the difference between empathic accuracy and empathy.
References
- Ickes, W. (1993). Empathic accuracy. Journal of Personality, 61(4), 587–610.
- Ickes, W. (1997). Empathic accuracy. New York, NY: Guilford Press.
- Ickes, W., Buysse, A., Pham, H., Rivers, K., Erickson, J. R., Hancock, M., Kelleher, J., & Gesn, P. R. (2000). On the difficulty of distinguishing “good” and “poor” perceivers: A social relations analysis of empathic accuracy data. Personal Relationships, 7(2), 219–234.
- Ickes, W., Gesn, P. R., & Graham, T. (2000). Gender differences in empathic accuracy: Differential ability or differential motivation? Personal Relationships, 7(1), 95–109.
- Schumann, K., Zaki, J., & Dweck, C. S. (2014). Addressing the empathy deficit: Beliefs about the malleability of empathy predict effortful responses when empathy is challenging. Journal of Personality and Social Psychology, 107(3), 475–493. https://doi.org/10.1037/a0036738
- Zaki, J. (2014). Empathy: A motivated account. Psychological Bulletin, 140(6), 1608–1647. https://doi.org/10.1037/a0037679
- Zaki, J., & Ochsner, K. N. (2012). The neuroscience of empathy: Progress, pitfalls and promise. Nature Neuroscience, 15(5), 675–680. https://doi.org/10.1038/nn.3085

